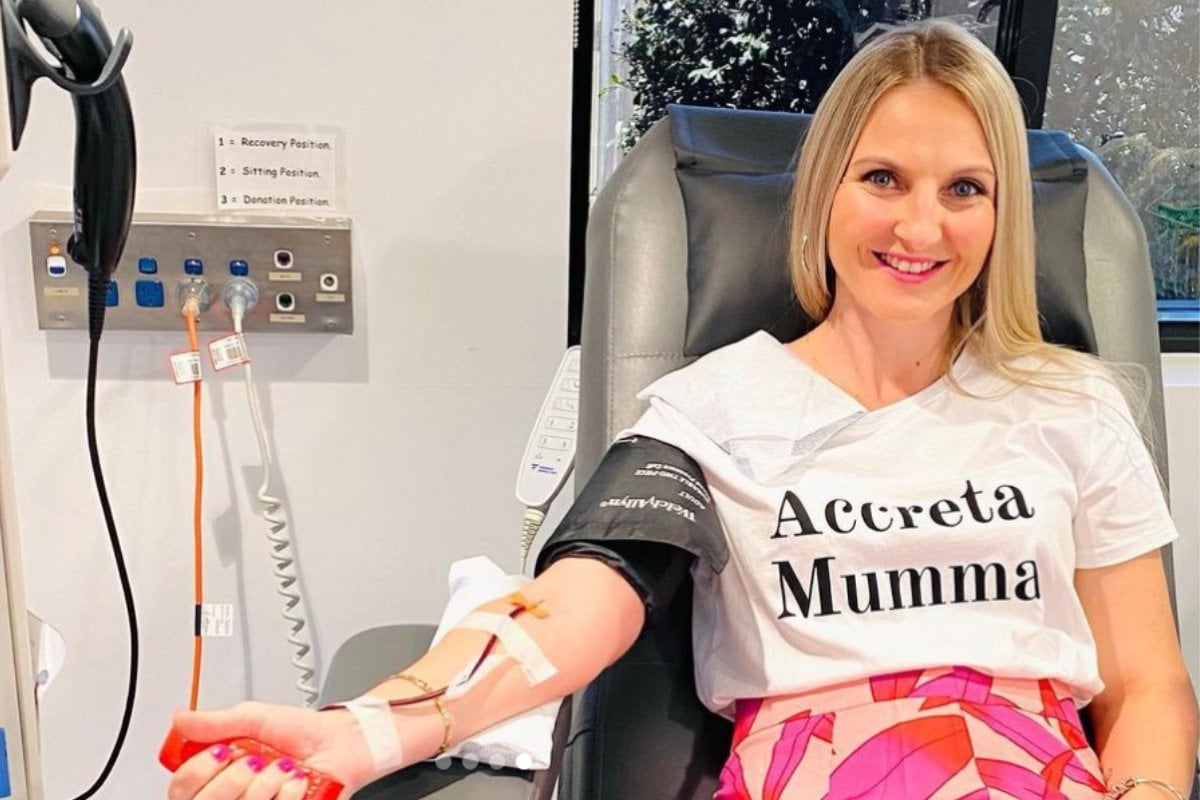
Talitha Jensen had been through the births of her two daughters, Mila and Arleigh, by the time she was pregnant with her third baby in 2018. While her first two pregnancies and births were not without some complications, she could never have expected the complex challenges she would face the third time she neared her due date.
"After my second c-section in 2014 for Arleigh, the specialist told my husband Brendon and I that if we wanted more kids, we should give my body a proper break to recover," Talitha tells Mamamia.
"We took the advice seriously and were so happy in 2018 to be pregnant again."
Watch: Bec Judd on c-sections. Post continues below.
At eight weeks, along Talitha began experiencing some bleeding. But a scan of her baby's heartbeat put her mind to rest. By 13 weeks, and again at 20 weeks, the scans were showing some blood flow issues that had doctors concerned.
"This was the first time anyone mentioned that I might have a rare condition called placenta accreta where the placenta is not working as it should be. I was referred for an MRI where they discovered it was actually placenta increta."
 Pregnant Talitha. Image: Supplied.
Pregnant Talitha. Image: Supplied.

