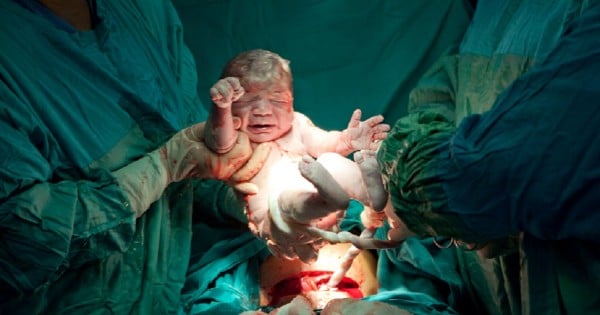
A submission to a UK health review by Hans Peter Dietz, a professor in obstetrics and gynaecology at the University of Sydney, suggests that the push to drive down caesarean rates may be contributing to an increase in injuries to women during forceps assisted deliveries.
As reported by The Motherish, “Professor Dietz’s team showed 81 per cent of women who had a forceps delivery suffered damage. The potential fallout from an attempt to reduce caesarean section rates included increasing rates of maternal pelvic floor tears from forceps deliveries, postpartum haemorrhages as a result of long second stage labours, and uterine ruptures in vaginal births after preview caesarean deliveries.”
This begs the question, what are we doing to women in the race to cut the number of caesareans?


Top Comments
I think that if everything looks good to your OBGYN, then attempting a vaginal birth is a good thing, but if you decide that isn't for you, the decision should be respected. I have had 2 vaginal/forceps births, both times with the babies in distress, an emergency c-section after a 26 hour labour(bubs was almost 10 Ib and it was 'cephalic disproportion', she was simply too big), and an elective c-section.
I would have to say that my elective was my best birth experience, although c-sections are harder, in general, to recover from that a 'good' vaginal delivery.
The tears I suffered after both my forceps deliveries, were excruciating. I tore badly all the way up vaginally with my first and had surgical repairs, and tore all the way in the other direction with my second and was doubly incontinent for a few days. NOT pleasant and quite depressing and distressing to go through...
My third, 26 hour labour, was my worst, and then I had to cope with the c-section(I was vomiting throughout), subsequent haemorrhage and blood transfusion, and then a Golden Staff infection. Horrendous. My 4th baby was born by elective c-section and it was a calm experience, where I was not physically exhausted before my baby was born, and it was my best birth experience, by far.
I would elect to do another planned c-section in a second, as it would obviously be the best experience for me, and for baby.
I am ending things at 4 healthy children, though...!
I ended up having a planned cesarean and found it to be a really good experience. I am small (55kg) and my husband's family all have huge heads. When the 20 week scan showed a large head I spoke to my ob, wait and see, some people with narrow hips have lots of give, hip size doesn't have anything to do with ability to birth and that of the head was engaged it would look good.
Come to the end of the pregnancy, head is still off the charts, and baby is looking big and head not engaged.
My ob gave me the risks and the option of both. These are the risks of c-section, these are the risks of vaginal birth. For me the risks to me and my baby (things like distress, getting stuck, shoulder diaplacia) were deal breakers to me.
Baby was delivered 10 days early at 10pound, head 97+%. I had a great recovery. If my next bub looks big I won't have any hesitation in having another elective c-section. And I'm a bit of a hippy, natural mum!